Why is the physical environment important for people with dementia?
Dementia is associated with progressive impairments of memory, perception, orientation, information processing, planning, sequencing, performing and monitoring actions, and communication. Therefore, cues that built in or are produced by the physical environment are more important for people with dementia than for cognitively unimpaired older adults. Ideally, the environment should compensate for deficits, maximise independence and support personal identity. Environmental features that have a particular impact include lighting, noise level, temperature, clarity, stimulation, and orientation.
What are the effects of an appropriate environment?
An appropriate design of the physical environment has a number of beneficial effects on people with dementia:
- Improving of quality of life
- Facilitating spatial and temporal orientation
- Supporting meaningful activities
- Enhancing social interaction
- Reducing changed behaviours such as anxiety and agitation
What is dementia-friendly architecture and design?
There are several principles of environmental architecture and design for people with dementia. A dementia-friendly building or flat should provide:
- A structure that is self-explanatory and easy to understand
- Controlled levels of background noise and visual stimulation
- Appropriate lighting and color contrasts
- Single rooms with individual and homelike character
- Individual items of furniture and other objects
- Specific, easily identifiable spaces for specific activities, e. g. cooking or leisure
- Short corridors and few decision points
- Well visible and easily accessible toilets
- Easily accessible and secure exterior spaces
What makes a home dementia friendly?
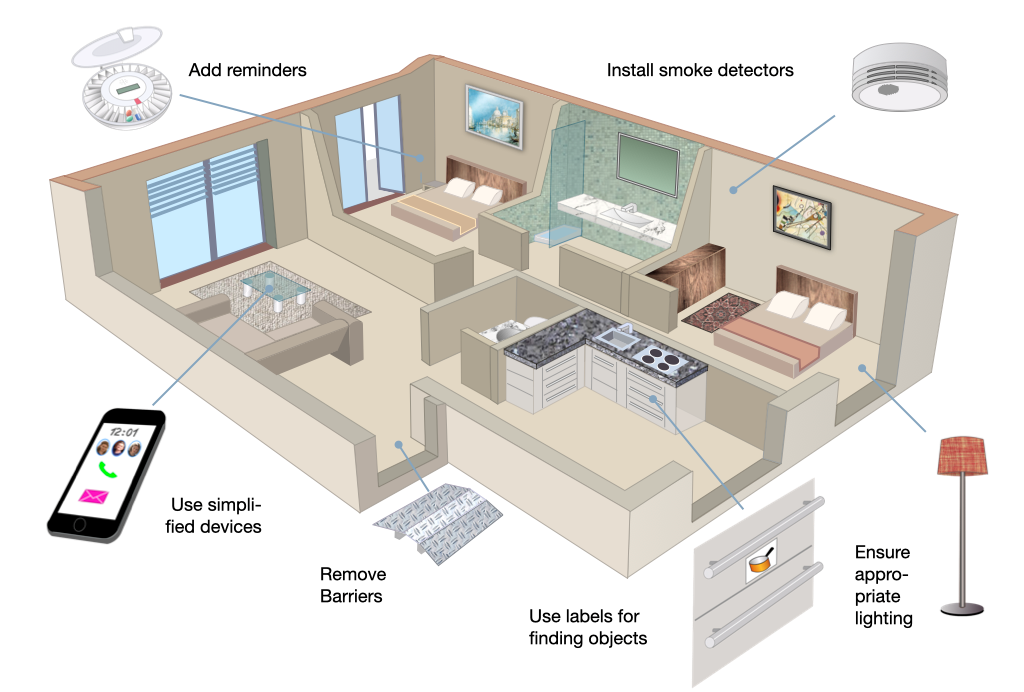
Suggestions for modifications inside the home
It is not advisable to make major changes to the home overnight, because the familiar environment is important for people with dementia to feel at home. However, there are simple things that can be done to help someone with dementia to continue living independently in their home.
- Improve lighting, particularly on stairs and in the toilet
- Automatic light sensors can make lights come on automatically when someone passes by
- Reduce glare, shadows, and reflections – they may be misinterpreted as water or people in the house
- Reduce excess noise, e. g. a radio or TV constantly playing
- Remove clutter, e. g. stacks of newspapers or boxes
- Allow manoeuvring with walker and wheelchair
- Use safer flooring, avoid rugs or mats on the floor – they may be misinterpreted as objects that need to be stepped over, which could lead to trips or falls
- Increase bathroom safety, e. g. by using a walk-in shower, a shower seat, or grab bars
- Use contrasting colours, e. g. for furniture that contrasts from walls and floors, or the toilet seat
- Remove troubling reflections, e. g. mirrors – they can cause confusion as people with dementia may not recognise themselves
- Use labels and signs, e.g. on cupboards and doors; use words or appropriate pictures or photos; see-through cupboard doors may be a great help to someone with dementia, as they can then see what is inside
- Provide information, e.g., using a large clock with LCD display – people with dementia may be able to read digital information about time better than traditional clock hands (see: assistive technology below)
Suggestions for modifications outside the home
- Facilitate entering the home, e. g. by safety railings on stairs
- Make sure that walking surfaces are flat to prevent trips or falls
- Outdoor spaces must be secure to prevent someone wandering off
- Raise flower beds to help people with restricted mobility look after their garden
- Provide sheltered seating areas to enable someone to stay outside for longer
- Use adequate lighting, e. g. for the garden entrance
- Automatic light sensors can make lights come on automatically when someone passes
Assistive technology
Assistive technology refers to devices or systems that support people with dementia to maintain or improve independence, safety, and wellbeing. Different kinds of assistive technology are available which address people with cognitive impairment or dementia and family carers.
The goals of assistive technology for people with dementia are:
- Ensuring safety inside and outside the home
- Supporting independent living, activity and quality of life
- Facilitate communication and social interaction
- Delivering treatment
- Keeping people with dementia cognitively fit
- Providing entertainment
Types of assistive devices for specific goals
| Goal | Type of device |
| Ensuring safety inside and outside the home | • Alarms (e.g. bed detectors, mats, fall detectors, movement detectors, physiological monitoring) • Fire, smoke, gas, flood detectors • Door and window sensors • Electronic door locks • Automatic lighting • Automatic shut-offs on household appliances • Person locators • Alarms (e.g. bed detectors, mats, fall detectors, movement detectors, physiological monitoring) |
| Supporting independent living, activity, and quality of life | • Reminders • Speaking objects, object finders • Timers, calendars, clocks • Remote controls • Robots |
| Facilitating communication and social interaction | • Simplified telephones, smart phones, telephone amplifiers • Tablet computer applications |
| Delivering treatment | • Medication dispensers |
| Keeping people with dementia cognitively fit | • Cognitively stimulating exercises • Exergaming |
| Providing entertainment | • Computer games • Digital photo frames • Artificial animals (Paro) • Reading devices • Social robots |
Examples of modifications inside and outside the home
Size and characteristics of the setting

Smaller settings with homelike characteristics are associated with higher involvement in activities, better functioning in activities of daily living, and slower decline functional abilities. A homelike atmosphere also enhances engagement and independence in activities. In special care units, a personalised, homelike design decreases aggressive behaviours and to increase time and engagement in common spaces. People with more privacy express less anxiety and aggression. Relocation of people from traditional settings to specialised care facilities improves quality of life and reduces agitated behaviours.
Lighting

Poor illumination produces dim or dark surrounding, uneven illumination creates shadows and uncontrolled glare. Lighting should be bright, windows should be large.
Walking surfaces
Avoid rough and uneven surfaces, strong patterns, and dark colours. Don’t use materials and finishes that produce glare and appear wet and slippery.
Stairs

Remove loose carpets, provide firm handrails, mark stair edges. Install a stairlift to enable access to upper floor.
Seating

Use strong constructions with appropriate height.
Bathroom safety

Use supportive technologies to ensure bathroom safety. A thermostatic care shower makes temperature control easy. There are also showers that automatically shut down after a certain amount of time to prevent flooding. Flood-proof plugs for baths and basins open up when a certain pressure is reached, allowing the water to drain away until the pressure is reduced, at which point they will close up again. In addition, a flood detector can be fitted which sends an automatic call to someone to help. However, prevention is usually a better choice than an alarm.
Image: Geberit Vertriebs GmbH
The bathroom should be equipped with a barrier-free shower, handrails, bath seats and non-slip bathmats. Bright or contrasting colours help the person use the bathroom facilities because they can see them clearly. Self-reflection in the mirror may be disturbing for a person with dementia and therefore should be avoided.
Other important safety adjustments are:
● no carpet in a bedroom,
● no glass table,
● darker coloured floor compared to walls.
Arrangement of objects

Remove unnecessary objects, simplify the environment, label objects, place objects purposefully. In the kitchen: increase visibility of objects that should be used, e. g. by glass-fronted wall units. Use objects with traditional design for better recognisability.
Cues

Use pictures as models and provide coloured cups to support oral care. A familiar tap design (e.g. cross-head taps) supports independent handwashing. Arrows and signs with the word „toilet“ and a picture can be effective in directing people with dementia to enter and use the toilet independently.
Image: Richter & Frenzel, Graefelfing, Germany
Outdoor design

Improve accessibility of the home by ramps with appropriate handrails.

Elevated flowerbeds provide better access into the garden for elderly people with mobility difficulties and allows them to continue pursuing their interests.
Images: 1) ALTEC GmbH 2) Private (AK)
Examples for assistive technologies
Digital door locks

Electronic Alzheimer’s proof door locks are an easy way to keep entryways securely locked during the night or while the caregiver is away. Packages usually include a knob and keypad. To unlock, someone needs to know the code which the caregiver has set on the system. Some systems come with a tampering alarm, which disables it for one minute and sounds an alarm if someone enters the wrong code multiple times.
Person locators

This watch has been specifically developed for people with dementia and their carers. The carrier of the watch can be spotted anytime and spoken to using the communication function of the device. The looks are those of a sports watch. The device can keep in range of emergency contacts, which are stored in the watch and notified if the SOS button was hit.
Object locators

These devices are useful for finding items around the home, such as keys, walking sticks or handbags. The beeper is attached to the object to be tracked. When in need to find it the corresponding letter on a remote control is pressed. The locator fob will then make a loud beeping noise.
Communication aids

This picture telephone automatically dials a number when the button showing the respective person is pressed. In the case of incoming calls, the corresponding buttons lights up.
Image: Audioline GmbH
Medication dispensers

Automatic pill dispensers can help a person safely take their medication at a set time of day. The devices are filled with tablets and programmed by the user or carer to dispense pills several times a day. Some pill dispenser feature an alarm and flashing light to remind users when to take their medication. They may also have a communication module which transmits text messages to designated contacts (e.g., family members) and an e-mail if medication has not been dispensed from the device at the appropriate time.
Image: courtesy of MEDIRING GmbH Ratingen, Germany
